Center of Excellence
Patent Foramen Ovale (PFO)
Program Overview
Our multidisciplinary team includes specialists in Interventional Cardiology, who perform minimally invasive procedures to close PFOs; Neurology and Stroke Medicine, who evaluate and manage neurological symptoms associated with PFO; Advanced Cardiac Imaging, which uses cutting edge technology to accurately identify heart defects; and Stroke Rehabilitation, providing comprehensive support for recovery and helping prevent recurrent events.
By combining state-of-the-art diagnostics with personalized treatment plans, we ensure each patient receives the most appropriate and effective care. Our mission is to improve outcomes and enhance quality of life through compassionate, evidence-based care tailored to individual needs.

What Is a PFO?
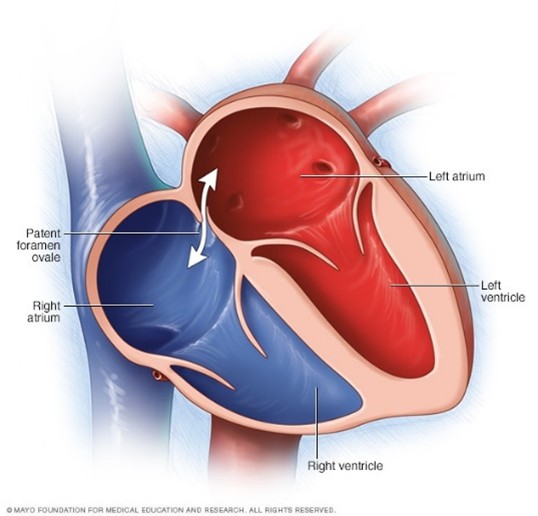
A Patent Foramen Ovale (PFO) is a small, flap-like opening between the heart’s upper chambers—the right and left atria—that typically closes shortly after birth. However, in about 25% of people, this opening remains partially or fully open, or “patent.”
For most individuals, a PFO causes no symptoms and often goes undetected. In some cases, though, it can allow small blood clots or air bubbles to bypass the lungs and travel from the right to the left side of the heart—potentially reaching the brain or other organs and leading to health complications.
Why Does PFO MATTER?
A PFO may be linked to several medical concerns, including:
- Cryptogenic Stroke – A stroke with no identifiable cause, possibly due to clots passing through the PFO.
- Transient Ischemic Attack (TIA) – A temporary blockage of blood flow to the brain, often called a “mini-stroke.”
- Migraine with Aura – Some research suggests a connection between PFO and migraines involving visual or sensory disturbances.
- Decompression Sickness – A risk for scuba divers, as bubbles may pass through the PFO.
- Low Oxygen Levels – In rare cases, a PFO can cause reduced oxygen in the bloodstream if blood bypasses the lungs.
Understanding your PFO and its potential impact is the first step toward informed decisions, peace of mind, and expert care.
Who Should Consider PFO Closure?
This procedure is most often recommended for patients who have experienced a stroke believed to be related to a Patent Foramen Ovale, or considered in other select situations.
PFO CLOSURE: What You Need to Know
For patients whose PFO has been linked to stroke or other significant complications, closing the PFO can be an effective way to reduce the risk of future events.
- The procedure is minimally invasive, performed by inserting a catheter into a vein in the leg.
- Through this catheter, a special closure device (shaped like a tiny umbrella or plug) is guided to the heart and placed across the PFO to seal the opening.
- Over time, heart tissue grows over the device, permanently closing the PFO.
- Most patients go home the same day or after a brief hospital stay, depending on individual circumstances.
- Recovery typically involves short-term anti-platelet medications and scheduled follow-up visits.
Testing and Diagnostics
To deliver precise and personalized care for patients with Patent Foramen Ovale (PFO), we utilize advanced diagnostic tools to confirm the presence of a PFO and evaluate its clinical significance. Common tests may include:
- Bubble Study (Saline Contrast Echocardiography): A specialized ultrasound that uses microbubbles to detect abnormal blood flow between the heart’s chambers.
- Transesophageal Echocardiogram (TEE): A high-resolution imaging test that provides detailed views of the PFO and surrounding heart structures.
- Brain MRI or CT scan: These imaging techniques help identify signs of previous strokes or other abnormalities that may suggest a PFO-related embolism.
- Long-Term Arrhythmia Monitoring: Devices such as Holter monitors, event recorders, or implantable loop recorders are used to detect atrial fibrillation or other irregular heart rhythms, helping determine whether a PFO is the likely cause of stroke.
- Hypercoagulable Workup: Blood tests that assess inherited or acquired clotting disorders which may increase the risk of stroke.
These diagnostic tools help guide treatment decisions and ensure each patient receives care tailored to their unique health profile.
Clinical Research Trials
We participate in ongoing clinical trials and research to improve PFO care:
GORE® CARDIOFORM Septal Occluder and Antiplatelet Medical Management for Reduction of Recurrent Stroke in Patients with Patent Foramen Ovale (PFO): the REDUCE Post Approval Study
Frequently Asked Questions
Is PFO closure safe?
Yes, PFO closure is a well-established procedure with a strong safety record, performed by experienced interventional cardiologists.
Will I need medication for life?
Typically, blood thinners are prescribed for a short period post-procedure; most patients do not require lifelong anticoagulation solely due to PFO.
Can PFO cause migraines?
Some patients with migraines with aura report improvement after PFO closure, but more research is needed for this sole indication.
What’s recovery like?
Most return to normal activities in a few days. You may need to take a blood thinner like aspirin for a few months.
Will I feel the device?
No, the device becomes part of your heart tissue. You won’t feel it or notice any difference in daily life
Is it covered by insurance?
In most cases, yes — especially if PFO is linked to a stroke. Our team can help verify your coverage.










